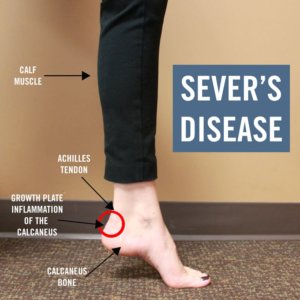
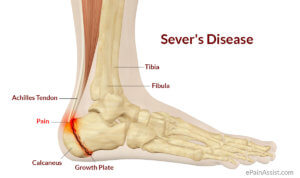
Sever’s condition (Calcaneal Apophysitis) is an inflammation of the growth plate of the bone at the back of the heel (Calcaneus bone).The condition usually affects children between the ages of 8 and13 years old and is more common in boys than girls. The prevalence is greater in highly active individuals during aggressive growth phases, but may affect any adolescent child during the active growing phase of the skeleton. In some individuals this can be episodic in nature or it may last for some time and then once settled, never return.
Presentation.
The pain is normally localised to the posterior aspect of the heel bone where the Achilles tendon attaches, although pain may be present under the heel or radiate up into the back of the calf muscle. Often the pain is experienced in one heel only, but it can also present bilaterally. Individuals who are engaging in general activities such as running, jumping or sports such as football, netball and basketball are more susceptible. Pain is often felt when the heel comes into contact with the ground and can be severe. Walking or running on the toes may reduce the symptoms. This is because strain is reduced across the plane of the epiphyseal plate, as the heel is raised off the ground. The area can be red and swollen but often the only sign of Sever’s is the child complaining of pain.
During the adolescent years the bones are still in a growth phase and the epiphyseal (growth) plates of the skeleton are not yet fused and fully ossified. This means that areas subject to excessive or repeated traction from strong tendons such as the Achilles can cause inflammation and pain at the point where they insert.
Another common site for this to occur is at the front of the knee with a condition called Osgood’s Schlatter’s. During rapid growth periods surrounding puberty these growth lines appear to be weakened further due to increased fragility of the cartilaginous growth plate. A combination of factors such as growth, poor foot function and biomechanics, insufficient support from footwear, or excessive training especially on hard surfaces may lead to the onset of symptoms.
Diagnosis.
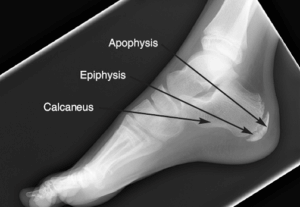
Sever’s condition is a clinical diagnosis which can be reached based on the medical history and presenting symptoms. A simple and effective test which can be done is the “Calcaneal squeeze test” which will identify localised pain symptoms. This will then need to be combined with a series of further tests to confirm the diagnosis including assessing the foot and ankle biomechanics for over pronation. X-rays may show sclerosis of the bone or fragmentation of the calcaneal tuberosity but these are not normally advocated unless the examination or presentation reveals a particularly severe presentation. MRI scans are not commonly used but may help rule out the possibility of calcaneal stress fractures or Osteomyelitis.
Prognosis.
The conditions of both Sever’s and Osgood’s Schlatters are self limiting and usually resolve with the correct advice and management. There seems to be some hereditary traits but we are still unsure why some adolescents develop it and others do not. There are often biomechanical reasons but it is usually caused by excessive amounts of sport, or rapidly increasing the individuals activity without taking into consideration the developing skeleton and whether this can take the loading being imposed upon it. If a child is good at one sport they often excel at others resulting in them participating in different sports, usually on a daily basis. The skeleton does not have sufficient time to rest and heel before it is expected to cope again with more load and stress, resulting in a reaction in the form of a pain full condition such as Sever’s.
Management and treatment.
- Activity modification is usually sufficient to control and settle symptoms.
- Non steroidal drugs and pain medications may be required to help with the pain but only for short periods.
- Local applications of Ice packs through a damp towel for up to 10 minutes per session can help with the pain from inflammatory conditions.
- Taping can offer relief and allow some participation in activity.
- Stretches and mobilisation of tight calf muscles can help but are best avoided in periods of acute flare up of inflammation.
- Immobilisation in a short leg walking cast may be necessary in particularly severe cases or when x-ray evidence of fragmentation is evident.
For further advice please do not hesitate to contact the clinic for a chat.